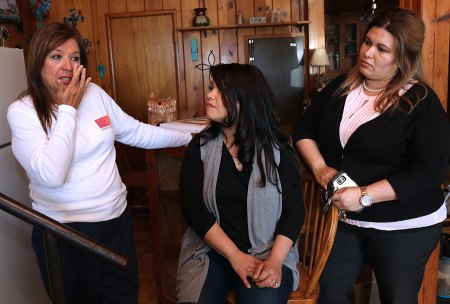Opioids don’t discriminate.
All levels of government have identified opioid abuse as a significant public health threat. The Washington Post reports that the opiate epidemic is killing hundreds of people a day, “akin to the 1918 flu pandemic.” The overdose crisis continues.
No community remains safe. Even in California and Kings County, where some may argue the epidemic hasn’t reached epidemic levels, we are beginning to feel the pain. As an editor and concerned citizen, I wanted to learn more about the role opioids play in our community.
The woman resting her slight hands on a large polished table in front of me is happy and confident. She has a handsome, radiant smile that easily puts those she talks to at ease, and as this opioid victim begins to tell her story, a self-assurance arises as she recites her emotional narrative – a verbal memoir spoken from the heart. Her story is an emotionally-charged account of despair, fear, failure, humiliation, struggle, and finally, a forthright, genuine tale of redemption and triumph.
Her story is like so many others who have experienced drugs. She is a survivor. Last year 60,000 Americans, like her, weren’t so fortunate.
Forty-year-old Josette Bejarano was once a victim – and then a blessed survivor. She was 32 years old, she said, an ambitious young woman from Selma, employed at PG&E, enjoying a “pretty good life” when things began to fall apart for her. It was then that her life took a downward spiral when she fell from grace, accidentally finding, and then succumbing, to opioids.
Her story has a happy ending. But that’s not always true for others, who, during their short lives, also have gone to war with drugs – and lost their battles. While Josette earned her battle-scarred victory, Hanford’s 23-year-old Amanda Mattos Sharp, an attractive young woman who as a child aspired to write for The New York Times, lost her battle against drugs on March 16, 2016. She died of a heroin overdose.
Amanda’s 18-year-old brother – because he was an adult at the time – was the first to learn of his sister’s death on that solemn day in March from law enforcement officials. Unfortunately, he was tasked with the painful duty of informing his mother that his sister, her daughter, had died, the victim of heroin.
“My son was at his dad’s house alone, and the coroner went there and told my son. My son had to be the one who had to come in and tell me,” remembered Ana Nicks, Amanda's mother. “He came into the bedroom; he’s crying and just frantic.” Her first thought was that something happened to his father. “He tells me it’s my daughter, and that’s when I was probably not consolable.”
Nicks told me her daughter’s story, a harrowing journey of concern, promise, rehabilitation, and then sadness.
Nicks is the human resources manager at Lemoore’s Leprino Foods, and inspired by her daughter, is working to create a “detox” facility in Kings County to help people like Amanda tackle the scourge of drugs. To this end, she sits on the Adventist Health Foundation Board and is a member of the Adventist Health’s Community Advisory Board where she advocates for stronger measures to battle opioid addiction.
Amanda went to rehab three different times. “She was the most beautiful I’ve seen her in a long time after her second rehab,” said Nicks. “We went through a lot of hard times as a family. How do we deal with this? What do we do? There’s no handbook that helps you get through it.”
Above all, there was concern, love, and patience. “I told Amanda you have to get out of this, you have to fight hard, or it’s going to kill you,” said an anguished Nicks. “Heroin addiction is one of the hardest if not the hardest to break. It’s a very ugly drug and so easy to get.”
Nicks said that Amanda’s funeral service was at the Church of Jesus Christ of Latter-day Saints in Hanford. The family could not locate a site for the service when the church’s gracious offer came to have it there. “The church was overflowing. This loss touched everybody in a very private way.
"Amanda was calling out for hope. At the time there were no facilities to take her in unless she was ‘clean,’” said Nicks. “Hannah’s House wanted desperately to help but was confined by its funding requirements. We have to create a system in this town where if another person’s family or friends are looking for help, here’s where you can go, here’s where you can get honest feedback.”
Amanda was born and raised in Hanford, a typical kid, said her mother. "She was active in everything. She was a good student, and she wanted to write for the New York papers, but mostly she wanted to have her own family and be a loving mom.”
It was in middle school that Ana began seeing changes in her daughter. “It was some time about the summer of eighth grade,” she remembered. “It started with marijuana. What I saw later as a parent was that the kids were messing with the stuff in their parents' medicine cabinet.”
Amanda started to get into trouble with probation. At the time Nicks was in the process of a separation from her husband, and she was entering high school. “There were a lot of things happening all at one time,” she said.
“Amanda always made friends with everybody, and she never judged anybody.” And like any other loving parent, Nicks warned her daughter not to associate with other kids suspected of using drugs.
“As a parent we all want children to surround themselves with perceived positive peers. But in reality, there are kids you never really thought were capable of doing drugs. There is no socio-economic class or anything that says that kids are going to do drugs or that kids are not going to do drugs.
“I knew my daughter was struggling, and I wanted to be educated.” Nicks attended seminars to learn more about the problem. “I tried to get educated. (She learned that) We have a much bigger problem, and we need to find ways to deal with it. We’re not protected just because we’re here in Hanford.
“The community (then) was not ready.” Nicks hopes that maybe, thanks to Amanda’s story, the community is ready to deal with the issue.
Amanda’s story inspired Nicks‘ fellow employees at Leprino to raise $23,000 through a golf tournament, individual contributions, and a matching $10,000 donation from the Leprino Foods Company Foundation. All donations were for Amanda’s Home (named for Nick’s daughter), one of several facilities operated by Champions to help kids like Amanda and Josette break the cycle of drugs.
Amanda’s Home is a sober residence for adult women, no matter what age, who need a safe and secure place to find refuge and beat back the opioid demons. Women can have their children with them as they are medically supported to help them with their substance abuse needs. Nicks supported the efforts of Champions to apply and license withdrawal management beds at both their male and female residential facilities (Hannah’s House and Samuel’s House). Photos of Amanda hang in the home, and posted in the house is her heart-wrenching handwritten letter to heroin. The poignant message helps others understand genuinely how big this demon is.
Amanda has been gone for nearly two years, and still, Nicks reflects on the challenges that faced her daughter as she struggled to cleanse herself of drugs. “When Amanda was in trouble with probation or cited for possession, she would appear in court. There, she would simply be released and told to sign up for drug classes and pay fines,” remembered her mother. “She needed help. I needed help.”
Prisons are full, prompting county jails to house prisoners meant for long-term incarceration. “So, kids and adults, who are struggling with substance abuse, are released to go back to what they were doing.”
Nicks says there must be a better way. “There needs to be a better system which allows repeat offenders to be rehabilitated,” suggesting that local jails be allowed to create mandated rehab sites to help with recovery. They could work in tandem with local rehabilitative agencies.
“My daughter once told me the longer you can stay clean, the stronger you become. But whether you get clean in jail or a rehab program, there has to be a collaboration with other agencies. Addicts need structure to help build their strength. They can’t be left to figure it out for themselves.”
Nicks said that without that support – from jails, local agencies, family - so many addicts go back to the drug life. They become homeless, commit crimes, or much worse.
And as society debates rehabilitation, the roll call of opioid victims is, unfortunately, climbing in the United States and California, and even closer to home in tiny Kings County.
What are opioids? If at some point in your life, you’ve had surgery, which in some cases might very well cause a certain degree of pain, a physician may have prescribed a painkiller. Common medications for pain include Vicodin, Percocet, and OxyContin. These drugs – and others – are derived from opium, a narcotic borne from the poppy, a flower used by humans for thousands of years.
It was common for physicians to prescribe painkillers. Ten years ago, after having my gallbladder removed, I was prescribed Vicodin, which the doctor indicated would relieve the pain. Fortunately, my pain wasn’t severe, and I discarded the drugs. But others, who end up accepting the drugs, are at risk of developing a dependency, which for some can lead to a very dark and confusing place.
Josette’s dependency on opioids began with a routine, harmless trip to the dentist, and it only ended when she said God spoke to her from the confines of a Kings County jail cell.
She was one of the lucky ones, escaping what for many addicts very well could have been a death sentence. Nearly 60,000 persons died from opioid overdoses in 2016.
As I listen to Josette’s story, I find it difficult to fathom that this striking, confident woman was once a victim of drugs. Well-worn images of drug addicts appear in my mind. Their faces are pitted and bearing scars, images of rotting teeth, a blank mug shot – an addict turning old before her time.
Sitting before me is a handsome woman with a bright smile and a confident bearing. Josette hardly looks the victim. The smile, her friendly demeanor, belies the notion that she was once – and still is – a statistic in the war against drugs. In her early forties now, Josette could easily pass for a much younger woman.
We meet in a stately downtown Hanford office building that once housed a well-known Hanford law firm, but now houses Champions, a faith-based, non-profit organization devoted to providing support to people like Josette, lost souls seeking welcome shelter from the tragedy of substance abuse and violence. Champions’ mission is to provide positive environments for those consumed by drugs or mental health issues. Its mission: to “put into order, disordered lives.”
The elegant office with its shiny table is occupied now by Dr. Crystal Hernandez, the organization's director, and one of Josette’s biggest boosters. Hernandez is a friendly face, who for the past five and one-half years as the agency’s executive director, has helped others just like Josette escape from their demons.
“We never turn anyone away,” said Hernandez, a native of small-town Avenal, explaining Champions’ mantra. “We meet people on the street … and we bring them in for treatment.”
Is Kings County a haven for opioid abusers? “A lot of our young people come into treatment at adult services here. One of the first things we do is access their use, their patterns. And surprisingly, a great number of teens that are 18 to 19 come into treatment are usually forced by their parents, or by the court, or by some other. They’re using heroin. There are a large number of individuals using heroin here locally,” said Hernandez, a trained psychologist.
“It’s the young age bracket that started with prescription medication. A lot of the 25 and under population will say that they engaged in ‘pharm parties’ because that’s the thing they do now,” she said.
“Your entrance to a party is a handful of pills. You put them all in a bowl, mix them up, and pull out a handful of skittles (pills).”
Most young people don’t have money to pay for prescription drugs. “What do they turn to? Their answer is heroin.”
Josette’s dark journey, an odyssey that ended with an addiction to heroin, began under similar circumstances. “I went in for some extensive dental work, and the dental work had to be done in stages, like an implant, a couple of crowns, things like that,” she remembered. “To be quite honest, all I needed was Ibuprofen, but the dentist gave me Norco. They can gauge how much pain you’re in, right? I started taking it, and the prescriptions just kept coming because the procedures were done in stages. It was over a long period of time, and through that period he continued to give me the Norco.”
Norco, for the uninitiated, is a controlled substance. It’s a pain reliever that medical experts say if misused, can lead to addiction and dependence. It can cause respiratory distress and death when taken in high doses or when combined with other substances, especially alcohol. Other brand names are Vicodin, Lorcet, Hycet.
And Josette, whose knowledge of the pain reliever was virtually nil, kept on getting the powerful pain reliever – again and again.
“I remember I loved it. I thought pain pills knocked you out. This made me feel empowered and euphoric. It made me productive. I started taking them more and more,” she said.
Her dentist would refill her prescription often as her dental work progressed. “By the time the dental work was done I found someone to buy them (pills) from.”
Thus began an odyssey of sorts that resulted in years of substance abuse that culminated with a two-month stretch in the Kings County Jail. It’s where she said God saved her life.
It was spiritual “warfare” for Josette. “First of all, I didn’t realize I could get physically addicted to it. I just knew that it was making me feel good. I would hear these things in my mind, that (said) well, if it were really bad then the doctor wouldn’t have prescribed it, to begin with; or you’re not taking too many because the doctor definitely wouldn’t be refilling you every time you called him if you abused it. You start to talk yourself into those things.”
Because she was working and had earned some money, she felt she could afford more pills, but when her supplier failed to provide her with additional opioids, Josette discovered the ugly side of her addiction. “I began to get sick. I began to get this doom and gloom horrible feeling. I didn’t know what was wrong with me until she (her friend) explained to me that all I needed to do was take a few more pills to feel better.”
It was probably at that point she realized she was an addict. “It was at that moment that everything changed for me, because – then and there – I realized I was stuck, and there was no turning back.”
For Josette though, the doom and gloom would disappear – when she discovered more pills.
At the time she was paying $5 a pill, and at the end of her Norco experience, she said she was consuming upwards of 40 pills a day. “I started incorporating more pills, other prescriptions into it, like Xanax, and Soma.”
After working six years for PG&E, she was laid off. “That’s really what prompted me to get treatment,” she said. “I knew I couldn’t afford my addiction anymore, and that’s kind of what catapulted me into the heroin addiction.”
She visited a pain specialist during that time because she felt “stuck” in her life, knowing full well she was dependent on drugs. “I didn’t see the light at the end of the tunnel.”
The pain specialist helped wean her off Norco with another medication called Suboxone, a drug employed to treat opioid addiction. “I’ve detoxed off of pain pills, and I’ve detoxed off of heroin several times, and the withdrawal from pain pills had me on my knees. It floored me. You would think heroin is worse, but the physical withdrawals from prescription medication, for me, were ten times worse. It was horrific, and it was the worst thing I’ve ever gone through in my life.
“You have major, major anxiety in your stomach to where you could almost see your stomach tighten up. You have this enormous sense of gloom and doom where you just feel hopeless. This is where I realized the full definition of desperation because you feel desperate.”
Hot and cold sweats were constant reminders of her addiction. She suffered irritable leg syndrome and more, describing her pain as a form of Chinese water torture. “You have no peace over any part of your body. You can’t even walk when you’re withdrawing (from) prescription medications. You feel like you’re going to die.”
Soon, heroin entered her life, and it wasn’t a positive relationship.
“During this time frame, my standards started to get lower. I started hanging around with people that I would never hang around with. Different characters began coming into my life, and one of the people I was hanging out with happened to have heroin. He was smoking it, and he asked me if I wanted to try it. I said sure. If you had asked me when I was growing up that I would end up a heroin addict, I would have said you were crazy.
“There was no way, but when you feel as though you’re already addicted to it and don’t know how that happened, you’re already stuck, then you feel like there’s really nothing to lose. Does that make sense, I know it sounds crazy? That’s how fast and easy something like that can sneak up on you.”
Heroin was a lot cheaper, she said. It was about $10 a day when Norco was $200. That was in the beginning she recalled. By the end, it was up to $50 to $100 a day.
At some point, Josette’s entire existence fell apart. “My life went up in flames. My friends couldn’t deal with it anymore.”
Her parents suffered too, but they helped her through treatment. But when she decided to return to drugs Josette’s actions left them at a loss. They refused to concede. They continued to check on her. “I was already in my thirties. What were they supposed to do? It was a very back and forth kind of thing for a long time.”
She was evicted twice and arrested more times than she could count for stealing – to pay for her addiction. “I started doing meth at that time as well. Once you do one, you start doing another. You just start to do everything."
She served felony probation in Fresno and Tulare counties when in 2015 she was arrested in Kings County. “They don’t mess around in Kings County,” she said. “I spent two months in jail. It was just enough time for me to detox, and for my mind to start clearing, but the judge said he wouldn’t release me. I’d have to go straight into treatment, and that’s how I ended up at Hannah’s House (a Champions-based women’s treatment facility for mental health and substance abuse).”
Her time in Hannah’s House taught her to live again, she said. “In jail, I had this God encounter, let’s say, where I literally feel like I was delivered from my addiction.”
She said she was ordered to drug programs in Fresno County too, but it didn’t work. “You have to understand the call of the drugs, and the call of that street life was so strong that nothing – other than God – was going to break that.
“I just know that when I left there (Kings County Jail), I was so grateful not to be in jail. It’s like he (God) gave me this willing spirit to be able to accept the conditions of this program. And then he started to raise the standards in my life. I realized that everything that I was learning at Hannah’s House – they taught me how to live again - reinforced the standards he was raising in my life.”
Just two months previously, Josette just wanted to be a heroin addict. “I didn’t want anything else.”
The drugs are gone, she said. She’s not even tempted. “I’ve changed every aspect of my life, and that all occurred while I was at Hannah’s House. Slowly Josette regained her existence and managed to grow spiritual roots. She fell in love with the community. She eventually rented an apartment and made the transition to a restored life, a new existence, far from the maddening crowd of drug addicts and pills.
She’s involved in the church now. “I live a good life now,” she said, “And my parents have their daughter back. We have such a wonderful, beautiful relationship.”
Josette was lucky if that’s what you want to call it. Others, even in tiny Kings County, haven’t been as fortunate. There were other prescriptive pills too, Xanax, Soma, and others. “You’re self-medicating.”
Josette’s story is familiar.
“That’s typical,” said Hernandez who has seen many like Josette come to Champions for help. She knows full well the life experiences of addicts like Josette. When the money runs out, addicts often revert to heroin, a much cheaper high.
But there is always hope – and help.
Josette and Amanda are not alone. According to the New York Times, drug overdoses are the leading cause of death for Americans under 50, and its increasing every year. Overdoses now kill more people than guns or car accidents. In 2015, roughly two percent of deaths – one in 50 – in this country were drug-related.
Opioid addiction is indeed a national problem, buoyed initially by the over-prescription of opioid painkillers, and while other states have higher per-capita addiction rates, California, based solely on its 40 million-plus population is one of the country’s leaders in overdose deaths. According to 2016 statistics supplied by the Centers for Disease Control and Prevention (CDC), California, with its large population ranks just behind Florida in the total number of opioid deaths with 4,654, but is well behind in per capita deaths (deaths per 100, 000 population), tucked between Kansas and Montana.
The drug crisis facing Americans in 2018 had its roots in the 1980s when the pharmaceutical industry began aggressively marketing drugs like OxyContin. More doctors prescribed more and more medications for patients seeking relief from pain. Eventually, more and more patients started using the drugs, and many grew addicted, either from prescriptions or from taking them recreationally.
As of 2017, the highest overdose rates were in Appalachia, the Rust Belt, and New England. West Virginia has the dubious distinction of having the highest per capita rate at 52 West Virginians per 100,000 population.
According to Hernandez Kings County experiences high rates of opioid overdose deaths, opioid overdoses inpatient hospitalizations, opioid emergency department visits, and higher prescription rates than the state average (per capita).
Kings County has a high per capita rate in California, despite having just 150,000 residents. In Kings County, there were six deaths per capita due to all opioid-related overdoses in 2016. In 2014 there were 8.4 opioid overdose deaths in Kings County, 12.4 overdose emergency department visits, and 19.8 overdose inpatient hospitalizations per 100,000 residents.
Data measured in 2015-16 indicates the drug of choice in Kings County remains methamphetamine, while Kings County rates of heroin use have increased above that of the state (20 percent in Kings County, 2.3 percent in California).
Kings County, at just 150,000 residents, had six deaths from opioid-related overdoses in 2016. Los Angeles County had 353 opioid overdose deaths, about a 3.2 average. Fresno County has a 7.1 per capita rate.
California Opioid Overdose Surveillance Dashboard
There are promising signs. The Center for Disease Control and Prevention (CDC) has issued guidelines recently recommending primary care providers avoid prescribing opioid painkillers for patients with chronic pain. The risks from opioids greatly outweigh the benefits for most people, said the CDC.
Doctors are reevaluating the use of opioids, screening those who may be candidates for painkillers.
Law enforcement agencies throughout the United States have employed the opioid antidote Narcan. “Narcan prohibits the opium from invading any other part of the body,” said Lemoore Police Sergeant Alvaro Santos, who oversees drug investigations for his department.
On Thursday, April 5, Surgeon General Jerome Adams, issued the office’s first advisory in 13 years. He called for more people to carry the opioid overdose antidote Naloxone, commonly known as Narcan.
He emphasized that “knowing how to use Naloxone and keeping it within reach can save a life.” He noted that the number of overdose deaths from prescription and illicit opioids doubled in recent years. In 2016 nearly 64,000 people died of drug overdoses.
Santos said all Lemoore officers now carry the antidote. All law enforcement officers in Kings County carry the inhalers. “It’s almost like an inhaler,” said Santos about Narcan. “It’s often shot through the nose. That’s how it’s administered.”
It was during a stint with the Kings County Narcotic Task Force that Santos began seeing a rise in drug use. “When I was there we started to see a rise in heroin abuse, drug trafficking. This issue has been going on for a while,” he said.
Santos said Lemoore officers have never used Narcan. “No officers have had to use it. Due to the uprise in the country and the nation, we’ve decided to issue them to our officers just in case it happens.”
Many law enforcement officials get training every year. Santos recently attended a week-long session provided by the California Narcotics Officers’ Association.
“(Drug) abuse is increasing,” said the Lemoore officer. “More drug dealers are selling heroin. We find out that most of the time the addicts started with prescription drugs. Because prescription drugs are controlled heavily, at some point, they can no longer get a refill. “
“They like to turn to other drugs, like heroin, to self-medicate. We had quite a few cases when I was on the task force.”
Opioids are costing us. But not just in lives lost or damaged. The White House Council of Economic Advisors estimates that the opioid crisis has cost this country $504 billion in 2015, or about 2.8 percent of that year’s domestic gross product. Other organizations say it could cost us more, trillions more in the long run.
Individuals and communities think Big Pharma – a conglomeration of pharmaceutical companies – should foot the bill. To that degree, cities, counties, Native American tribes and unions are suing companies that manufactured and distributed powerful painkillers. The lawsuits argue that the companies should pay for the damage the drugs brought to their citizens and their communities.
The lawsuit contends that the cost of governing in the age of opioids has rapidly expanded as opioids overwhelm communities faced with the mounting costs of jails, education, foster care, and more.